 |
|
|
|
Derek Maylor, NW BT Unions H&S Co-ord member and Health & Safety Officer (Telecom section) of the CWU's Grter Mersey Amal Branch; reports on a Royal Society Of Medicine webinar, looking at Long Covid:
Our understanding of Long Covid is ever changing but the data is collated in too many different ways making comparisons difficult. Over 90% of people with symptoms of Long Covid never required hospital treatment and only had mild symptoms. People have had respiratory problems after Covid that they never had when they were ill with Covid. Fatigue and chronic chest pain being consistent symptoms and we are quickly learning about the use of current medication in treating symptoms, for example common antihistamines can help lessening respiratory issues. A study by Matta J, Wiernik E et al (2021) "Association of self-reported COVID-19 infection and SARS-CoV-2 Serology test
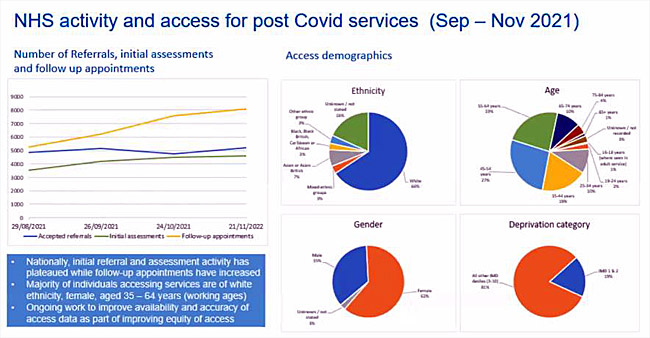
Above was the initial NHS plan, now developed into the current plan which is via the GPs front door with help to coordinate services to patients (see over) – noting the huge importance of looking after NHS staff.
There is now ever improving rehabilitation for people with Post Covid Syndrome along with integrated recovery pathway including both the physical aspect as well as an in-depth psychological assessment and intervention for all ages. There are in person physical and virtual/digital options for recovery with occupational health support and vocational rehab where appropriate. The early patient and staff feedback shows most patients report significant improvement in quality of life and ability to return to (near full work. There are studies and information such as https://theconversation.com/heres-where-and-how-you-are-most-likely-to-catch-covid-new-study-174473 available to communicate the Long Covod risk in different settings or age groups for example.
There is support from the voluntary and care sectors to address health inequalities and make connections beyond healthcare, disseminating good practice, raising awareness to improve quality particularly for those from marginalised or disadvantaged communities. There is a commitment in the NHS Long Covid Plan 21/22 to partner with national charities as well as VCSE organisations to unify delivery. With ongoing learning there are emerging themes on access and quality which we are always looking to improve as we are all further educated across every health sector. Going forward there is a further £90, announced for 22/23; Integrated Care Systems have been requested to support primary care in their pathways including sharing knowledge with other ICS and to implement actions to mitigate inequality of access to services. Clinical core requirements include access to diagnostic testing, access to multi professionals’ teams, access to rehab pathways and offer of face-to-fae wherever possible. Professor Roz Shafran is the Chair in Translational Psychology at the UCL Great Ormond Street Institute of Child Health and spoke about care for children and young people, about a third of which have been affected which is extremely high rate and a surprise, this is even when the child has very few or no symptoms. Children are recovering and the future is positive, paediatric clinics are not experiencing in depth problems or hospitalisations. Lt Col Mark Cranley spoke about the effects on the UK military, he is the armed forces expert for Consultant Rehabilitation and Sport & Exercise Medicine at Defence Medical Rehabilitation Centre. Although the military have history on rehabilitation treatments, like elsewhere in NHS, Covid was a learning curve; now much of what is offered is patient education and coping mechanisms. Statistically 80% to 90% of patients have returned to work which worryingly means that up to 20% do not, this is also from a younger demographic than the general population, also generally a fitter healthier grouping. An in-depth paper is available from www.ncbi.nlm.nih.gov/pmc/articles/PMC8180841/ Susanne Nielsen is the World Health Organisation Consultant in Rehabilitation and based in WHO European Office. There are various approaches to Long Covid, and priorities change across the EU but there is an acceptance that the condition exists and requires more research. There is a leaflet from WHO website that has been translated into over twenty languages to assist, this has become the starting point for the EU members. Even when the pandemic ends, Covid being declared by the WHO as over, Long Covid will continue, it will still need investment and research like any post viral condition.
Going back to work may mean looking at what work can be done by someone and not what used to be done by them pre Covid, things may never return for some patients but does not mean they are not a valuable worker.
The day concluded with the usual near statuary a panel chaired by Tom Moberly, UK Editor of the British Medical Journal and consisted of Dr Bola Owolabi, Director, Health Inequalities, NHS England and NHS Improvement; Dr Graham Burns, Consultant physician, Lecturer, Royal Victoria Infirmary and Newcastle University, National Specialty Adviser for Long Covid, NHS and Darren Brown, Specialist Physiotherapist, HIV and Oncology, Chelsea and Westminster Hospital NHS Foundation Trust. Two years into the pandemic and the vison NHS set out to keep equality as prime concern has been maintained but despite all the effort there are still problems which we must continue to address, there is a disproportionate access form the most disadvantaged – though that is not criticism of the NHS. There is much greater visibility and there are specialist clinics for Long Covid (though none in Scotland). Some of the challenges were already in the NHS have been highlighted, we already knew that some ethnic minorities have a slower take up of services even when offered in a similar demographic in white ethnic groups. A serious concern for clinicians is social media which has made some people experts because they have read something on Twitter, we cannot be swayed by public opinion but by scientific fact. Moving forward future guidelines need to advise services on providing specialist rehab for those patients that have neurological dysfunction, not just cognitive but physical. There are a small number of patients who present with movement disorders where no specific cause is found but Covid infection is identified as the catalyst, such neurological rehabilitation is a specialism, and some patients needs access to these therapists. There appears to be many similarities with chronic pain, particularly functional disorders, which have traditionally been underfunded with an undue emphasis on interventional and pharmacological treatments, this precedent may impair the provision of healthcare for patients with long covid in some parts of the country. We are seeing a high correlation with fatigue and brain frog, as the patient learns to manage their fatigue through rehab the brain fog improves.
|


 Graham Lawton, Staff Writer at New Scientist opened the day with Dr Elaine Maxwell the former Scientific Advisor at NIHR being the first speaker.
Graham Lawton, Staff Writer at New Scientist opened the day with Dr Elaine Maxwell the former Scientific Advisor at NIHR being the first speaker. 

 Lesley Macniven is a writer, Coach and OD Consultant, Long Covid Support Leadership Team and Employment Group Chair and organised a support group.
Lesley Macniven is a writer, Coach and OD Consultant, Long Covid Support Leadership Team and Employment Group Chair and organised a support group.